Newly graduated medical professionals struggle to adapt to the realities of hospital life. Many experience significant stress, which impacts their careers and often forces them to leave the profession. In this article, we’ll examine the key indicators that lead to adaptation problems and how to address them. Despite the depth, commonality, impact on medical professionals, groups and social roots of the issue, this topic still remains under-researched.
Medical School and their culture
After the lengthy study process at medical school, when it comes to applying their knowledge in practice, medical student level of preparation for real-life work leaves much to be desired. The expectation is that after completing basic training and beginning internship at a hospital, students should be prepared for relative independence, which will prepare them for residency. However, the level of student readiness is not universal.
Regardless of country or medical school, research shows that the problem of unpreparedness for clinical work is widespread. For example, the article “Preparedness for Practice: The Perceptions of Medical Graduates and Clinical Teams” (Med Teach, 2012, UK) compares data on the stated and actual levels of readiness for independent work among medical school graduates. It turns out that the differences between students within a single university are significantly greater than the differences between universities overall. This means that the level of preparation depends not on a specific institution or curriculum, but on how to conduct medical education as a whole.
The authors emphasize that students tend to overestimate their own readiness level. This is particularly evident in their skills in receiving and handing over patients, as well as in teamwork. Even if a student has excellent academic achievement, he or she is often unprepared for the real workload and are forced to deal with their problems on their own.
One less obvious factor that influences autonomy is the culture of the medical school. The training of physicians and nursing professionals varies greatly, due to the specifics of the industry as a whole and to the policies of specific educational institutions. In the United States, for example, future physicians are often nurtured in a collegial atmosphere, while nursing professionals face a competitive environment and psychological pressure. (Why this happens is a separate, larger topic.)
There are proven practices for fostering a healthy culture in medical schools, but their implementation is far from ideal. Medical students, when faced with a challenge, often avoid seeking help from mentors or colleagues for several reasons: stress is disorienting, there’s a fear of revealing one’s ignorance, mentors discourage feedback, and a widely accepted standardized, “impersonal” approach to student problems.
- The level of preparation does not depend on the university, but is linked to the upbringing and shortcomings of the medical education system.
- The stated readiness for independence of graduates is overestimated.
- The prestige or status of an educational institution does not guarantee better graduate readiness.
First steps towards autonomy
It’s often forgotten that autonomy begins with understanding one’s role in a new environment. It’s assumed that a healthcare professional, having acquired academic knowledge, should intuitively understand how to act in a given situation. But in a real hospital setting, it’s not always clear how much responsibility can be assumed and when it’s necessary to yield to the supervision of a mentor.
Autonomy is an important factor in a hospital setting, as a new medical professional must be able to:
- Make an accurate diagnosis;
- Choose the most effective (or least harmful) course of action;
- Formulate treatment plans and communicate them to others; (if these are mid-level medical personnel, then it is necessary to be able to independently follow the treatment plan and establish clear communication with the attending physician, colleagues, and support staff);
- Recognize in advance that it is necessary to seek help from more experienced colleagues: sometimes this time frame could be a matter of minutes.
For medical professionals, it is important to remember that they don’t exist in isolation: the presence of colleagues and mentors in a hospital play a crucial role. However, new graduates may encounter obstacles, such as bullying, hazing, authoritarian mentoring style based on the principle “I’m the boss, you’re the idiot”, or a negative reaction to initiative in situations that require more experience than may seem. These factors increase disorientation and cumulative stress during the transition to practical work.
Key sources of difficulties
- Uncertainty about one’s role in a new environment
- Absence of support from colleagues
- Absence of a reliable mentor
Autonomy and organization: time = money!
Another important factor influencing autonomy of healthcare workers, in general, is the specific nature of how healthcare institutions operate. A hospital differs from a true business or administrative institution in that it combines two aspects — healthcare and bureaucracy — that should seem to work synergistically. In practice, however, this interaction often generates conflicting environments in which business processes are given center stage and the medical component takes a back seat. The primary source of such conflict is hospital profitability and the quality of patient care: the goal to get more patients and perform more procedures without increasing the number of staff, the lower the quality of provided care.
In this situation, physician autonomy is especially important. Administration demands quantity over quality: filling out countless forms, maintaining electronic records, completing continuing education courses and corporate compliance modules takes a significant amount of time and attention. Nevertheless, if a physician makes a mistake due to a heavy workload, the responsibility falls solely on them. It is not always obvious that true autonomy depends not only on the preparedness and level of the professionalism, but also on the system within which medical professionals work.
Numerous studies have attempted to address these structural issues by granting healthcare workers more autonomy while simultaneously improving the quality of care. However, the results are limited: autonomy is a complex, nonlinear phenomenon that cannot be easily provided.
The authors of the article “Sink or Swim: Near-Peer Teaching Eases the Transition into Hospital-Based Medical Education” (Med Teach, 2015, UK) describe how “baptism by fire” forces young professionals to gain the trust of their colleagues by prematurely taking on more responsibility and pushing the boundaries of their established practice. While this might facilitate adaptation, it carries risks for both patients and the healthcare professionals alike. Situations will evolve spontaneously, without any reliable or proven strategies.
Moreover, physician autonomy is influenced by the type and size of the organization. The larger the hospital, the more difficult it is to adapt.
- The type of organization and its size influence the autonomy of healthcare professionals.
- Healthcare professionals do not always conflict with the institution and can benefit from its functions without losing their autonomy.
- Autonomy is a function of many factors, not all of which are obvious.
In the article “Physicians’ Perceptions of Autonomy Across Practice Types: Is Autonomy in Solo Practice a Myth?” (Soc Sci Med, 2014), author Professor Katherine Y Li demonstrated that physicians working in large institutions have perceived lower levels of autonomy compared to their colleagues in smaller practices. The reasons for this include high workloads, logistical constraints, and strict requirements for reporting. Ultimately, even a high level of expertise does not give physicians a sense of independence, and actual work is often not reflected by the compensation.
- Collaborating with management doesn’t always mean a loss of autonomy, and sometimes it even offers benefits.
- A clear connection must be established between the time a healthcare professional can devote to a patient and the perception of autonomy relative to the size and type of practice.
Communication between instructor and student
A young medical professional’s career depends largely on the quality of their mentor. Mentors aren’t always motivated for their role: teaching students is rarely rewarded with additional pay, and instructors are often required to teach as a “duty.” If there are too many students per mentor, the quality of their practice declines. In many cases, students effectively act as a hospital staff, which increases the responsibility and stress of the inexperienced doctor or nurse.
Only tacitly acknowledged that a mentor can shape a future medical student’s perception of the profession for life. Negative experiences lead to anxiety and panic, which interfere with higher mental functions and increase the risk of errors that can jeopardize the patient’s well-being and in some cases lead to sentinel events. With proper support and a “safety net,” everything changes: even simple situations could become a training of confidence for the student. Knowing that one can ask for help without being humiliated and do their best without toxic criticism develops the ability to remain calm in stressful situations.
There’s an unspoken understanding that a mentor can set a future medical professional on a trajectory that will shape their perception of the work for the rest of their lives. For example, many medical professionals (both doctors and nurses) when faced with a high-paced situation of CPR can suddenly become extremely anxious without any apparent reason. Panic makes it difficult to adequately assess the situation, decreasing reaction time and disrupting communication and feedback loops, so a fairly straightforward procedure of resuscitation can lead to injury or death of the patient.
(How to help new grads overcome “stress imprinting” and what techniques help maintain composure is a separate topic. It is important to mention here that the quality of feedback plays a decisive role.)

Source: Scrubs, Season/Episode: Season 3, Episode 13 (“My Porcelain God”)
In the aforementioned article “Sink or Swim,” the authors emphasize that not only the content but also the form of feedback matters—tone, manner of speech, use of jargon, clarity of written comments, and detail of annotations.
It is crucial for students to have the opportunity to participate in debriefing, development of assessment criteria and peer review of practice. Even “imperfect” feedback from a peer at the moment of error can be more effective than “perfect” criticism from a mentor a week later.
- The instructor and student have a hierarchical relationship; student adaptation depends on good feedback from the mentor and colleagues.
- Feedback is not a monologue, but a complex process consisting of complex social mechanisms.
- Students are always interested in feedback, even if it is not outwardly obvious.
- Feedback between both student and instructor, and between students, must be synchronized.
- Feedback systems of the medical team require separate study.
Sink or swim
The lack of adequate training procedures for adaptation to working in a hospital setting leads to a situation where drowning persons could only try to save themselves. This is most often encountered by nursing staff. In nursing schools, there’s a repeated saying: “Nurses eat their young.” It reflects a deep-rooted culture of hazing, excessive demands, and poorly concealed hostility toward students and colleagues, trainees are assigned as a burden to experienced staff.
As a result, newcomers begin their careers with a “sink or swim” environment. This atmosphere hinders the development of autonomy, perpetuates feelings of vulnerability, and contributes to fast professional burnout.
- Newcomers begin their careers in a “sink or swim” environment.
- Hazing is a common problem in the medical field.
Mental health of medical students
Medical education and practice can be powerful sources of stress. Many causes of stress cannot be addressed at the individual level; the burden is cumulative and undermines mental health. Numerous studies exist on hazing, burnout, and toxic workplaces in medicine, but the recommendations are often superficial and trivial. The key problem is not only the toxicity of the environment itself but the fact that this fact is getting ignored: when the system doesn’t acknowledge the problem, finding a solution becomes impossible.
Some characteristic aspects:
- Burnout begins during the academic years and hinders future autonomy.
- Normalization of hazing hinders the development of practice.
- Dullened sensitivity to the patient turns a living person into an “object,” which exacerbates burnout.
- Mental health help for students should begin from the earliest stages of education.
It’s difficult to explain to someone outside the medical field what it’s like to work in such an environment. Medical staff face pain, suffering, misunderstanding, emotional storms, and responsibility for people’s lives, with decisions that must be made in seconds. Many students and young doctors struggle to cope with such a workload, especially when faced with conflicts at the workplace.
It’s important to understand that this is a problem of the system, not an individual. Support programs for medical students show limited success and rarely address their real, long-term needs.
Effective programs, according to the researchers, should include studying how to improve communication with hospital administration, how to expand mentoring and career planning services, and how to ensure students and young medical professionals have access to mental health specialists. And so on.
- Burnout at the school hinders future healthcare workers from gaining autonomy in real-world practice.
- Student mental health impacts their ability to achieve autonomy, so it should be a focus early in their education.
- University programs have shown results in helping students overcome nervousness, anxiety, and depression.
- There are no specific recommendations for addressing the causes and consequences of burnout, and recommendations for improving mental health are formulaic.
Death Simulator
Any student in the medical profession must be able to withstand the stress required to make critical decisions in situations where a patient’s life is at stake. But the question of what constitutes an “acceptable level” of stress remains unanswered.
One training method is the so-called “death simulator”: an artificially created training situation in which, even if the student does everything correctly, the patient still dies. The simulation is almost indistinguishable from real clinical practice. Its goal is to teach future physicians to maintain sobriety, objectivity, and the ability to analyze mistakes and cope with failures. This is an important skill: in real practice, doctors will inevitably encounter similar scenarios.
The purpose of the “death simulator” is to push students out of their “comfort zone,” where they are protected by mentors and colleagues. But not everyone can handle this type of training. Debates about the method’s benefits continue. Some studies even document an increase in anxiety in students after such training. Whether this is a good thing remains an open question.
Although future doctors undergo a variety of similar training sessions, the level of psychological stress is difficult to assess. Lack of knowledge and hesitation are clear risk factors. But the perception of stress itself is individual and difficult to measure.
- Psychological stress is not always measurable and can’t be adequately addressed. There are currently no reliable metrics for assessing and regulating academic stress.
- How to balance autonomy and support for medical students remains an open question.
- The perception and experience of stress, even in simulation conditions, can vary from person to person, and the adaptation process takes varying amounts of time.
Impact of social factors
All of the above factors that shape medical professional life are not just a result of the interaction between person and medical profession. They stem from broader cultural norms that start to take effect at the upbringing, general educational system and social life. Social habits, group dynamics, and motivations that develop in society become the building blocks of corporate culture that guide medical professional careers.
It is not obvious which qualities of medical students at all levels impact all metrics that we use to evaluate healthcare outcomes. But it is evident that educational standards are just a part of medical professional success in the industry.
One of the more often discussed aspects is motivation to join the healthcare workforce. There’s an example of many studies that ask “Why have you joined the medical field?”, that present predominantly altruistic motivations. However, any medical professional will recognize that this is not a whole story. Many students (one study suggests that up to 75% in the USA) are motivated by “income, security, and status”, answers that are most often revealed through an indirect style of questioning.
However, there are also signs of hidden disparities in the medical student demographic. More often, pecuniary motivated students come from high income families and have relatives with high medical degrees, but there’s also studies of a high rate of burnout due to debt-related stress of medical professionals that acquired student loans. They become ever more difficult to manage with stagnating compensation rates. Heightened demand to perform, results in high patient load and increasing rate of unnecessary procedures, that take a toll on intrinsic motivation and mental wellbeing of doctors (not to mention a devastating economic impact on the overall healthcare system).
The problem runs ever deeper when it comes to mid-level personnel. Often from low-income households, nurses become the highest paid members of their families, which becomes motivation for others to join nursing for “employment security”. Nevertheless, there’s a very high dropout rate (18% after the first year and up to 50% after the second year in the field) and struggle to retain nurses in the profession in general. Many core reasons such as bullying, sink or swim introduction to profession, lack of qualified leadership, general feeling of underappreciation and low compensation rates are well known, however remain unaddressed.
These factors are indirect, yet they produce cumulative effects on the environment and function of healthcare as a whole, and can’t be mitigated by a single policy or change of leadership.
Many of the precursors of current problems are rooted in the social factors that form our communities and interpersonal relationships, create our motivations and future outlook.
Our approach to culture, education, and healthcare management need to be completely revised.
Everyday life in medicine
A career in the medical field is not for everyone. In recent years, the number of applicants to both medical schools and nursing colleges in the United States has been declining. The COVID -19 pandemic accelerated this trend, with more and more professionals leaving the field or taking early retirement. This results in a severe shortage of personnel and increasing workload for newcomers and those who remain.
Students begin their internships in an environment where they are treated like full-fledged staff and immediately thrown into emergency situations—a common part of hospital life. Any confusion, uncertainty, or mistake takes its toll on the understaffed teams and becomes grounds for harsh criticism from senior colleagues. Being scolded at staff meetings is so commonplace that it’s now accepted as the norm. But this is precisely what accelerates burnout, creates and amplifies toxic culture.
Even with an excellent mentor and a supportive team, the hospital environment itself can be traumatic for a newcomer. Without mental preparation for the real world, it’s extremely difficult to sustain its pace and remain mentally stable. Stress, relatively easy access to narcotics administered in the hospital setting (and additional social factors) contribute to the rise of drug addiction among medical professionals.
A typical example of the stressors of the medical field is the 2019 New York Times article “I Remember the First Time I Witnessed a Teenager Die,” in which a medical student describes his experience in his third year. This text has become a kind of “standard” for discussing burnout, even before young doctors gain autonomy. (image below from the article).
- There’s no good approach for introducing students to the “everyday life of the hospital.”
- Burnout among new medical professionals is left to its own devices.
- Most medical professionals who decide to leave the profession do so within the first two years of work.
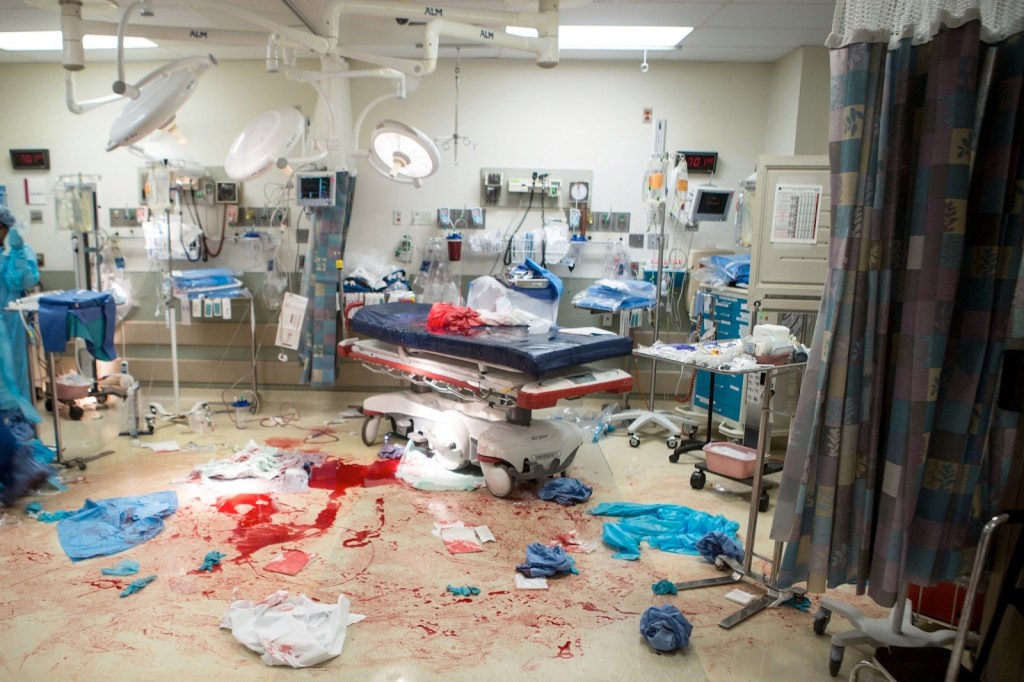
Source: TNYT, 2019.
Conclusions
Despite its relevance and scale, the topic of medical students’ adaptation to hospital reality remains underdeveloped.
- Medical schools do not purposefully prepare students for challenges of practice.
- The transition to autonomy occurs spontaneously and individually.
- The influence of the organization and type of medical institution on the process of autonomy development is often ignored.
- Medical and professional schools do not always foster a culture of collegiality and support, and rarely consider how workload affects the psychological state of students.
- Immersion in the “everyday life of medicine” is often too abrupt.
- Mentors and instructors are not always motivated, so the quality of feedback suffers.
- The accumulation of unresolved problems creates a toxicity within medical teams.
- The mental health of new grads receives insufficient attention.
- The systemic nature of these problems influences the decision of healthcare workers to leave the profession.
Recommendations
Stereotypical perceptions of the “new role” of healthcare professionals should be reexamined; prepare medical students and nursing staff for more complex team functions; establish clear rules for communication and feedback between doctors and nurses.
Create reliable statistics and develop tools to measure physician readiness; analyze barriers and develop mechanisms to overcome them.
Develop a strategy for training specialists that eliminate hazing practices, but maintain a productive level of stress.
Establish a clear link between the time a healthcare professional can devote to a patient and their perception of autonomy depending on the size of the practice.
Engage students in work groups by reducing barriers to receiving systemic feedback.
Sources
- Kopel J. J. Sir William Osler: A forerunner of mindfulness in medical practice. Proc (Bayl Univ Med Cent). 2019 Jun 10;32(3).
- Lin K. Y. Physicians’ perceptions of autonomy across practice types: Is autonomy in solo practice a myth? Soc Sci Med. 2014 Jan;100:21-9.
- Marshall S.D. Sink or swim? The difficulty of finding the correct level of independence and support for trainees. Br J Anaesth. 2015 May;114(5).
- Morrow G., Johnson N., Burford B., Rothwell C., Spencer J., Peile E., Davies C., Allen M., Baldauf B., Morrison J., Illing J.. Preparedness for practice: the perceptions of medical graduates and clinical teams. Med Teach. 2012;34(2).
- Obregon M., Luo J., Shelton J., Blevins T., & MacDowell M. Assessment of burnout in medical students using the Maslach Burnout Inventory-Student Survey: a cross-sectional data analysis. BMC Med Educ. 2020 Oct 21;20(1).
- Young J. B. Does Osler’s Aequanimitas Inform Our Contemporary Pursuit of Stillness? AMA J Ethics. 2022 Dec 1;24(12)
- Ziff O.J., Samra M. Sink or swim: Near-peer teaching eases the transition into hospital-based medical education. Med Teach. 2015;37(6).
- Yang, A., Langness, S., Chehab, L. et al. Medical students in distress: a mixed methods approach to understanding the impact of debt on well-being. BMC Med Educ 24, 947 (2024). https://doi.org/10.1186/s12909-024-05927-9 (2024)
- Glauser W. Do students enter medicine for money and prestige or to be of service? CMAJ. 2018 Feb 26;190(8):E229-E230. doi: 10.1503/cmaj.109-5560. PMID: 29483335; PMCID: PMC5826713. (2018)
- SortSmart Candidate Selection Inc.: Medical school admissions practices in the U.S. more likely to select applicants motivated by status, financial gains, and familial pressure to pursue medicine and may result in bias against applicants from lower income levels. (2018)
- Jon Helgheim Holte, Trine Kjaer, Birgit Abelsen, Jan Abel Olsen, The impact of pecuniary and non-pecuniary incentives for attracting young doctors to rural general practice, Social Science & Medicine, Volume 128, 2015, Pages 1-9, ISSN 0277-9536,
- Hassan M, Shahzad F, Waqar SH. Seeking motivation for selecting Medical Profession as a Career Choice. Pak J Med Sci. 2020 Jul-Aug;36(5):941-945. doi: 10.12669/pjms.36.5.2799. PMID: 32704268; PMCID: PMC7372692.
- Worthless back surgeries are a nagging pain for U.S. health care (2024)
- Survey Shows One-Third of Physicians Considering Leaving Medicine (2025)
- A Typical Week for First-Year Medical Students (2024)
- Why Nurses Quit and Leave the Profession (2023)
- Clinician burnout: poisonous to patient care, but preventable (2024)
- How to Prevent Burnout & Reach Your Medical School Goals (2024)
- I Remember the First Time I Saw a Teenager Die (2024)
- Sink or Swim. We need to reconsider how we train our doctors to be sure that they acquire the skills they will need
- The Current Landscape of Medical Student Burnout (2024)
- Young scientists flail in sink or swim system (2024)
- 8 ways to cut medical student burnout (2024)
Editor – Marat Kayumov

















